Is this Study a Step Closer to Migraine Blood Tests?
A new study has led to a flurry of media interest in blood tests for migraine. But what is the study really telling us?
The study was published online this month in the journal Neurology. 52 women with episodic migraine were in the study, along with 36 controls. Each woman had a blood test, which was checked for a group of lipids (molecules including oils, fats, and waxes) which regulate inflammation in the brain.
 The results were actually quite remarkable. Certain lipids, known as a ceramides (waxy lipids), were low in women with episodic migraine. Women with migraine tended to have less than 60% the ceramides of the controls. The more ceramides, the lower the risk of migraine.
The results were actually quite remarkable. Certain lipids, known as a ceramides (waxy lipids), were low in women with episodic migraine. Women with migraine tended to have less than 60% the ceramides of the controls. The more ceramides, the lower the risk of migraine.
Two other lipids were the reverse – higher levels meant an increased risk of migraine.
So would it be possible to tell who has migraine just from a blood test? Well, the researchers tried it, taking 14 of the participants at random and doing a blood test – and yes, they were able to tell who had migraine and who did not.
The immediate question is – of what use is that?
Frankly, these women already knew they had migraine – the symptoms are a dead give-away.
This study raises some of the same benefits and challenges as other research already has.
First, is a blood test really going to be more useful in diagnosing migraine than a few specific questions? Probably not in the near future. But what if the test could differentiate types of migraine, or differentiate between migraine and other headache disorders? Now we may have something useful.
Another question is – why these differences in lipid levels (or whatever the difference may be in a given study)? Is this being caused by migraine? Or migraine medication? Or is it part of the biology that leads to migraine in the first place? Could migraine be predicted – even prevented?
Back in 2011 we discussed another type of blood test for migraine. This test seemed to show a possible trigger, related to high levels of an amino acid known as homocysteine. In this case, people with certain levels may benefit from a specific treatment (for example, taking certain B vitamin supplements).
That’s not an overall test for migraine, but it’s useful for some people.
This most recent study was very small, and is not going to lead to immediate changes in treatment or testing. More studies need to be done to confirm the results, and perhaps most importantly to compare different types of migraine and other headache disorders such as cluster headache.
But this line of research could lead to more easy ways to customize treatment in the future.
Read more about the study in this press release from the American Academy of Neurology: A new marker for migraine?


 Now that you’re awake, the headache lasts for a few minutes – but could even last up to four hours.
Now that you’re awake, the headache lasts for a few minutes – but could even last up to four hours.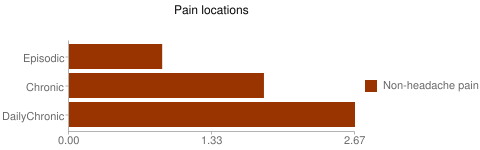 So the more chronic the disease, the more pain locations (see study at
So the more chronic the disease, the more pain locations (see study at  For each non-cephalic pain location, patients with episodic migraine were 30% more likely to progress to chronic. For patients who were already chronic, each pain location increased their odds by 6% to stay chronic. Read more at
For each non-cephalic pain location, patients with episodic migraine were 30% more likely to progress to chronic. For patients who were already chronic, each pain location increased their odds by 6% to stay chronic. Read more at 
 In this case, the connection was quite clear. While taking the medication (participants took it over a period of 10 days), the patients were much likely to ovulate – much less likely.
In this case, the connection was quite clear. While taking the medication (participants took it over a period of 10 days), the patients were much likely to ovulate – much less likely. Acetaminophen / paracetamol is a common drug to try first. In the case of migraine, intravenous magnesium may be tried as well.
Acetaminophen / paracetamol is a common drug to try first. In the case of migraine, intravenous magnesium may be tried as well.