The Best Medication for Migraine? The AHS Reports
Last month the American Headache Society came out with a new report suggesting which drugs have the best evidence behind them when it comes to migraine. According to the trials, what works the best?
 This, of course, does not mean that these medications will work the best for you. There is a lot of variation within migraine, and your doctor will help you decide where to start.
This, of course, does not mean that these medications will work the best for you. There is a lot of variation within migraine, and your doctor will help you decide where to start.
However, if your doctor isn’t talking about some of the treatments at the top of the list, you should be asking some questions.
The full report can be found here: The Acute Treatment of Migraine in Adults: The American Headache Society Evidence Assessment of Migraine Pharmacotherapies. However, here is a summary of some of the authors’ findings.
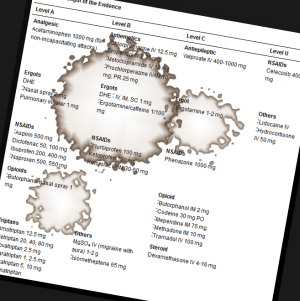
The medications with the best evidence behind them included:
- The Triptans: Certain specific triptan medications were mentioned, such as almotriptan, sumatriptan, and naratriptan
- Butorphanol nasal spray
- NSAIDs: aspirin, diclofenac, ibuprofen and naproxen
- Acetaminophen, but only for “non-incapacitating attacks”
- DHE
- Acetaminophen/aspirin/caffeine combo
- Sumatriptan/naproxen combo
Some of the medications that really don’t have good evidence behind them, or the evidence is conflicting at this time, include:
- Lidocaine IV
- Celecoxib
- Hydrocortisone IV
This is only a portion of the list – most medications fall between these two extremes. Also, it’s important to note that the researchers noted actual dosages, which means of course that any particular medication may work better/worse at a different dosage, but it may not have been studied.
Also, remember that these are only “acute” medications – taken at the time of an attack – not preventatives.
The conclusion of the study offers an appropriate warning:
According to this systematic review of the literature and structured grading of the evidence strength, specific medications within the following classes are considered “effective” for the acute therapy of migraine: triptans, ergotamine derivatives, NSAIDs, opioids, and combination medications. Several other medications are considered “probably effective” or “possibly effective.” This evidence base for medication efficacy should be considered along with potential medication side effects, potential adverse events, patient-specific contraindications to use of a particular medication, and drug-to-drug interactions when deciding which medication to prescribe for acute therapy of a migraine attack.
