James
Posts by James Cottrill:
Warning Signs of Migraine in Children
It can be a tremendous challenge to recognize migraine in children. We’ve talked a lot about symptoms in the past, and if you want a quick review, see this infographic – Does my Child have Migraine? and for more detail, 18 Reasons to Suspect Migraine in Your Child.
A few years ago we talked about a study on “Premonitory” Symptoms of Migraine in Children. That is, what are the warning signs that a migraine attack is starting?
 A new study has been done, on the same topic. So let’s take a look.
A new study has been done, on the same topic. So let’s take a look.
The new study confirms that it was common in children to have two “warning signs”, although the number varied. In fact, 85% reported two or more. The most common signs were (most common first):
- Fatigue
- Mood changes
- Neck stiffness
- Yawning
- Changes in concentration
This fits well with what the past study told us. Fatigue was reported in both as a top sign. “Irritability” was in the earlier study, and that would be included with mood changes here.
Of the top three in the earlier study,”face changes” was a commonly reported premonitory sign in children.
These symptoms not only help children and parents know that a migraine attack is starting, they may also help to confirm the migraine diagnosis. In fact, premonitory symptoms were reported in children as young as a year and a half old!
An interesting side note. The most common childhood episodic syndrome associated with migraine was a history of infantile colic. You can read more about migraine and colic here. 31% of these children had had colic.
You can read the full results of the study here: Characterising the premonitory stage of migraine in children: a clinic-based study of 100 patients in a specialist headache service
Note: One of the study authors was Dr. Peter Goadsby, who will be a speaker at the Migraine World Summit 2017. Get your free tickets to view the event online here.
Migraine and TMD: A Complex Relationship (that should not be ignored)
Although it’s not news that there’s a relationship between migraine and TMD, it might be a surprise just how complex the relationship is.
TMD refers to temporomandibular disorder/dysfunction, actually a group of disorders that affect (but are not necessarily caused by) the temporomandibular joint (TMJ) and surrounding muscles, nerves, and tissues. TMD may be caused by an injury or a disease such as arthritis. There may also be a connection with structural issues, and even clenching and grinding of the teeth while you sleep.
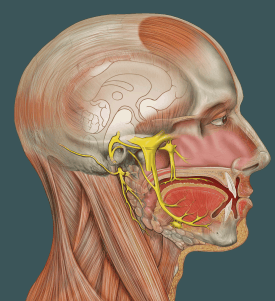
A 2016 study concluded that the connection between migraine and TMD was complicated further because of other physical symptoms, and the presence of bruxism (clenching/grinding teeth during sleep). Researchers concluded that doctors need to treat both headache/migraine and TMD together.
A study earlier this year asked the question – can the presence of headache disorders, such as migraine, actually predict TMD? In other words, even though migraine may/may not directly cause TMD, does the presence of migraine or another headache disorder tell us that the patient has a good chance of getting TMD later on?
The answer was yes. Patients who had no sign of TMD, but who did have a headache disorder, were far more likely to end up with TMD. The headache condition also tended to worsen in patients who eventually had TMD symptoms. Patients frequently ended up with migraine and TMD.
Researchers again affirmed what I mentioned in our last podcast – headache conditions, migraine in particular, need to be treated (Migraine and Generalized Anxiety Disorder). If they aren’t, they may lead to other conditions. One of those conditions is TMD. And what if the presence of new TMD in turn worsens the migraine? That could may migraine more difficult to treat.
The relationship between TMD and migraine is complex. It’s not a simple case of one causing the other. There may be underlying causes of both.
Doctors and patients need to focus on treating both, and being aware of changing and worsening symptoms so they can be caught early. If migraine or TMD are ignored, or just treated with “painkillers”, patients may find themselves with more pain in the end.
Podcast: Migraine and Generalized Anxiety Disorder
[display_podcast]
The main article we discussed was Adults with migraines have triple the prevalence of generalized anxiety disorder from ScienceDaily.com. You can read the abstract of the actual study here: Untangling the Association Between Migraine, Pain, and Anxiety: Examining Migraine and Generalized Anxiety Disorders in a Canadian Population Based Study.
Check the Mayo Clinic for more on generalized anxiety disorder symptoms.
I didn’t mention this other article, but there’s an interesting related study, also from the University of Toronto: Research shows dramatic link between inflammatory bowel diseases and anxiety disorder
And the article I mentioned about the Migraine World Summit: The Unexpected Reason You Should Pay Attention to the Migraine World Summit
Why Migraine Attacks may make you withdraw Into Darkness (or, Your Brain on the Holodeck)
Migraine attacks often come with a number of unwanted symptoms besides just pain. While some types of headaches may just be annoying, or others may make you want to pace the room, migraine patients generally retreat into darkness. And sometimes a migraine attack warning signal is – yawning! Why is that?
In a small study (Dopamine D2/D3 imbalance during migraine attack and allodynia in vivo), researchers at the University of Michigan discovered that, for these patients, dopamine levels fell during the attack itself.
A little background. These 8 patients had episodic types of migraine, and their brains were scanned both during the migraine attack and in between attacks. During the attack, researchers elicited an allodynia experience (sensitive, painful skin. See so that they could also see changes in dopamine levels when this symptom was present).
Dopamine molecules have a lot of functions in the body, such as influencing movement. But they’re most famous for the way they can make you “feel good” – motivating you to do certain things; rewarding and reinforcing behaviour.
The migraine patients had pretty normal levels of dopamine in between attacks – but when an attack hit, levels dropped.
So when dopamine levels crash, what happens? Well, you can guess. This may partly explain why you want to withdraw, get into a dark room, and stay still (although the pain may keep you moving). And the longer you’ve suffered from migraine, the worse your body seems to get at keeping your dopamine levels up where they should be.
Researchers also discovered that the dopamine levels fluctuated during the attack. When the patients felt the sensitive pain of allodynia, dopamine levels rose – but not back to normal levels. Unfortunately, this probably wouldn’t help you “feel better” – the partial rise would only be a reaction, possibly causing more symptoms, such as nausea.
Changing dopamine levels may actually be telling your body something valid – as Dr. Alexandre DaSilva (one of the researchers) put it: “This dopamine reduction and fluctuation during the migraine attack is your brain telling you that something is not going well internally, and that you need time to heal by forcing you to slow down, go to a dark room and avoid any kind of stimulation.”
In the emergency room, patients are sometimes given dopamine antagonists such as metoclopramide to help stop the wild fluctuations (and stop nausea).
Also, magnesium (taken to prevent migraine, but also given intravenously in emergency) may help keep levels stable.
(By the way – one of the topics of this year’s World Migraine Summit will be Calming the Hypersensitive Migraine Brain with Dr. Todd Schwedt of The Mayo Clinic)
The connection between migraine and dopamine levels isn’t a new discovery. What is new is the increasing ability to accurately see how levels rise and fall.
 And that brings us to the fun part of the study.
And that brings us to the fun part of the study.
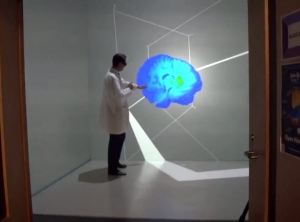
Here you can see Dr. DaSilva with a floating brain on his “holodeck”. Ok, it’s not exactly a holodeck, but it is an amazing way to see a brain – in this case a collection of responses from a number of brains – in 3D. It’s an incredible way to investigate the results of studies like this one.
For more information, and to see a video of Dr. DaSilva using the 3D brain, check out Brain scans show dopamine levels fall during migraine attacks.
via: Why Migraines Make You Tired and Sad: New Research Points to Role of Dopamine
