10 Highlights from the past 3 Months (September 2015 edition)
It’s always interesting to see which posts have been most popular with you, our community. This time around, it was very clear that four topics had jumped far up ahead of any other. So I’m going to post a little summary of the first four (actually, five) so that you can see what has generated all the interest, before you click through for the full story.
As usual, the three posts with the most Facebook likes are in bold. This is still a top ten list, even though it only goes to 9 – two posts are lumped together. 🙂
- The Migraine Brain: Very “Connected” – a brand new study is giving us insights into how the brain of someone with migraine is different, and how this may explain key migraine symptoms.
- Dizziness – Migraine – Could they be Dysautonomia Symptoms? and Dysautonomia and Migraine – do you feel weak, dizzy or faint when standing up or lying down? It could be a sign of an underlying condition that is making your migraine symptoms worse.
- A Review of Icekap – Icekap has generated a LOT of interest. It’s a new product that applies an old non-drug therapy for migraine in a new and up-to-date way.
- Botox and CGRP – and the Future of Migraine Treatment – treatments related to CGRP are perhaps the hottest thing in migraine research today. Could our study of Botox treatment and CGRP treatment provide a key to better “customized” treatment of migraine in the near future?
- Headache Waking You Up? Could Be Hypnic Headache.
- Are we ruling out hemicrania continua too soon?
- Are Solar Flares Giving Me A Headache?
- Is Your Medication Being Absorbed? Gastroparesis and Headaches
- Warning Flag: Do you have non-headache pain?



 The results were actually quite remarkable. Certain lipids, known as a ceramides (waxy lipids), were low in women with episodic migraine. Women with migraine tended to have less than 60% the ceramides of the controls. The more ceramides, the lower the risk of migraine.
The results were actually quite remarkable. Certain lipids, known as a ceramides (waxy lipids), were low in women with episodic migraine. Women with migraine tended to have less than 60% the ceramides of the controls. The more ceramides, the lower the risk of migraine. Now that you’re awake, the headache lasts for a few minutes – but could even last up to four hours.
Now that you’re awake, the headache lasts for a few minutes – but could even last up to four hours.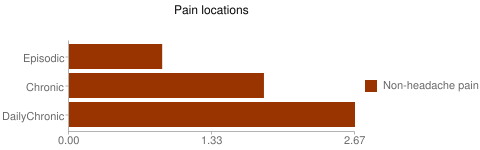 So the more chronic the disease, the more pain locations (see study at
So the more chronic the disease, the more pain locations (see study at  For each non-cephalic pain location, patients with episodic migraine were 30% more likely to progress to chronic. For patients who were already chronic, each pain location increased their odds by 6% to stay chronic. Read more at
For each non-cephalic pain location, patients with episodic migraine were 30% more likely to progress to chronic. For patients who were already chronic, each pain location increased their odds by 6% to stay chronic. Read more at 
 In this case, the connection was quite clear. While taking the medication (participants took it over a period of 10 days), the patients were much likely to ovulate – much less likely.
In this case, the connection was quite clear. While taking the medication (participants took it over a period of 10 days), the patients were much likely to ovulate – much less likely.